
Back وذمة وعائية Arabic Angioedem BS Angioedema Catalan Quinckes ødem Danish Quincke-Ödem German Αγγειονευρωτικό οίδημα Greek Angioedema Spanish آنژیوادم Persian Ɓutto FF Angioödeema Finnish
| Angioedema | |
|---|---|
| Other names | Angiooedema, Quincke's edema, angioneurotic edema |
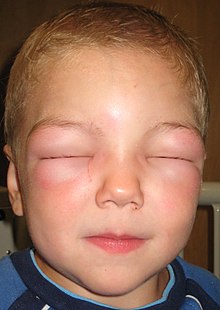 | |
| Allergic angioedema: this child is unable to open his eyes due to the swelling. | |
| Specialty | Allergy and immunology, emergency medicine |
| Symptoms | Area of swelling[1] |
| Usual onset | Minutes to hours[1] |
| Types | Histamine mediated, bradykinin mediated[1] |
| Risk factors | Family history[2] |
| Diagnostic method | Based on symptoms[2] |
| Differential diagnosis | Anaphylaxis, abscess, contact dermatitis[2] |
| Treatment | Intubation, cricothyroidotomy[1] |
| Medication | Histamine: antihistamines, corticosteroids, epinephrine[1] Bradykinin: C1 esterase inhibitor, ecallantide, icatibant, fresh frozen plasma[1] |
| Frequency | ~100,000 per year (US)[1] |
Angioedema is an area of swelling (edema) of the lower layer of skin and tissue just under the skin or mucous membranes.[1][3] The swelling may occur in the face, tongue, larynx, abdomen, or arms and legs.[1] Often it is associated with hives, which are swelling within the upper skin.[1][3] Onset is typically over minutes to hours.[1]
The underlying mechanism typically involves histamine or bradykinin.[1] The version related to histamine is due to an allergic reaction to agents such as insect bites, foods, or medications.[1] The version related to bradykinin may occur due to an inherited problem known as C1 esterase inhibitor deficiency, medications known as angiotensin-converting enzyme inhibitors, or a lymphoproliferative disorder.[1]
Treatment to protect the airway may include intubation or cricothyroidotomy.[1] Histamine-related angioedema can be treated with antihistamines, corticosteroids, and epinephrine.[1] In those with bradykinin-related disease a C1 esterase inhibitor, ecallantide, or icatibant may be used.[1] Fresh frozen plasma may be used instead.[1] In the United States the disease affects about 100,000 people a year.[1]
- ^ a b c d e f g h i j k l m n o p q r s Bernstein, JA; Cremonesi, P; Hoffmann, TK; Hollingsworth, J (December 2017). "Angioedema in the emergency department: a practical guide to differential diagnosis and management". International Journal of Emergency Medicine. 10 (1): 15. doi:10.1186/s12245-017-0141-z. PMC 5389952. PMID 28405953.
- ^ a b c Caterino, Jeffrey M.; Kahan, Scott (2003). In a Page: Emergency medicine. Lippincott Williams & Wilkins. p. 133. ISBN 9781405103572. Archived from the original on 2017-09-10.
- ^ a b Habif, Thomas P. (2009). Clinical Dermatology E-Book (5 ed.). Elsevier Health Sciences. p. 182. ISBN 978-0323080378. Archived from the original on 2017-09-10.
© MMXXIII Rich X Search. We shall prevail. All rights reserved. Rich X Search