
Back عطيفة صائمية Arabic عطيفه صائميه ARZ Campylobacter jejuni Catalan Campylobacter jejuni German Campylobacter jejuni Spanish Campylobacter jejuni Basque کامپیلوباکتر ژژونی Persian Campylobacter jejuni French Campylobacter jejuni HE Campylobacter jejuni Hungarian
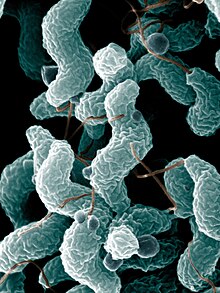
| Campylobacter jejuni | |
|---|---|
| |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Campylobacterota |
| Class: | "Campylobacteria" |
| Order: | Campylobacterales |
| Family: | Campylobacteraceae |
| Genus: | Campylobacter |
| Species: | C. jejuni
|
| Binomial name | |
| Campylobacter jejuni (Jones and Little, 1931) Veron & Chatelain, 1973
| |
Campylobacter jejuni is a species of pathogenic bacteria that is commonly associated with poultry, and is also often found in animal feces. This species of microbe is one of the most common causes of food poisoning in Europe and in the US, with the vast majority of cases occurring as isolated events rather than mass outbreaks. Active surveillance through the Foodborne Diseases Active Surveillance Network (FoodNet) indicates that about 20 cases are diagnosed each year for each 100,000 people in the US, while many more cases are undiagnosed or unreported; the CDC estimates a total of 1.5 million infections every year.[1] The European Food Safety Authority reported 246,571 cases in 2018, and estimated approximately nine million cases of human campylobacteriosis per year in the European Union.[2] Campylobacter jejuni infections are increasing at an alarming rate in Europe, North America, and Australia. In Africa, Asia, and the Middle East, data indicates that C. jejuni infections are endemic.[3]
Campylobacter is a genus of bacteria that is among the most common causes of bacterial infections in humans worldwide. Campylobacter means "curved rod", deriving from the Greek kampylos (curved) and baktron (rod). Of its many species, C. jejuni is considered one of the most important from both a microbiological and public health perspective.[4][5]
C. jejuni is commonly associated with poultry, and is also commonly found in animal feces. Campylobacter is a helical-shaped, non-spore-forming, Gram-negative, microaerophilic, nonfermenting motile bacterium with a single flagellum at one or both poles,[6] which are also oxidase-positive and grow optimally at 37 to 42 °C.[7][8][9][10] When exposed to atmospheric oxygen, C. jejuni is able to change into a coccal form.[11] This species of pathogenic bacteria is one of the most common causes of human gastroenteritis in the world. Food poisoning caused by Campylobacter species can be severely debilitating, but is rarely life-threatening. It has been linked with subsequent development of Guillain–Barré syndrome, which usually develops two to three weeks after the initial illness.[12] Individuals with recent C. jejuni infections develop Guillain-Barré syndrome at a rate of 0.3 per 1000 infections, about 100 times more often than the general population.[13] Another chronic condition that may be associated with campylobacter infection is reactive arthritis.[14] Reactive arthritis is a complication strongly associated with a particular genetic make-up. That is, persons who have the human leukocyte antigen B27 (HLA-B27) are most susceptible. Most often, the symptoms of reactive arthritis will occur up to several weeks after infection.[4][15]
- ^ "Campylobacter: Questions and Answers". U.S. Centers for Disease Control and Prevention. 2019-12-20. Retrieved 2020-01-02.
- ^ "Campylobacter". European Food Safety Authority. Retrieved 2 January 2020.
- ^ Fischer GH, Hashmi MF, Paterek E (2024). "Campylobacter Infection". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 30725718. Retrieved 2024-02-29.
- ^ a b "Campylobacter jejuni | Campylobacter Food Poisoning". www.about-campylobacter.com. Retrieved 2016-04-18.
- ^ Gundogdu O, Wren BW (March 2020). "Microbe Profile: Campylobacter jejuni – survival instincts". Microbiology. 166 (3): 230–232. doi:10.1099/mic.0.000906. PMID 32228803. S2CID 214750673.
- ^ Balaban M, Hendrixson DR (December 2011). "Polar flagellar biosynthesis and a regulator of flagellar number influence spatial parameters of cell division in Campylobacter jejuni". PLOS Pathogens. 7 (12): e1002420. doi:10.1371/journal.ppat.1002420. PMC 3228812. PMID 22144902.
- ^ Ryan KJ, Ray CG, eds. (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. ISBN 978-0-8385-8529-0.
- ^ "Online Bacteriological Analytical Manual, Chapter 7: Campylobacter". Food and Drug Administration.
- ^ Gorbach SL, Falagas M, eds. (2001). The 5 minute infectious diseases consult (1st ed.). Lippincott Williams & Wilkins. ISBN 978-0-683-30736-8."Multiple Campylobacter Genomes Sequenced". PLOS Biology. 3 (1): e40. 2005-01-04. doi:10.1371/journal.pbio.0030040. PMC 539341.
- ^ Perez-Perez GI, Blaser MJ (January 1996). Baronm S (ed.). Campylobacter and Helicobacter (4th ed.). Galveston (TX ): University of Texas Medical Branch at Galveston. ISBN 978-0-9631172-1-2. PMID 21413331.
- ^ Crushell E, Harty S, Sharif F, Bourke B (January 2004). "Enteric campylobacter: purging its secrets?". Pediatric Research. 55 (1): 3–12. doi:10.1203/01.PDR.0000099794.06260.71. PMID 14605259.
- ^ Fujimoto S, Amako K (June 1990). "Guillain-Barré syndrome and Campylobacter jejuni infection". Lancet. 335 (8701): 1350. doi:10.1016/0140-6736(90)91234-2. PMID 1971411. S2CID 38312888.
- ^ McCarthy N, Giesecke J (March 2001). "Incidence of Guillain-Barré syndrome following infection with Campylobacter jejuni". American Journal of Epidemiology. 153 (6): 610–614. doi:10.1093/aje/153.6.610. PMID 11257070.
- ^ "What is Reactive Arthritis?". Reactive Arthritis. 2019-02-06.
- ^ Allos BM (April 2001). "Campylobacter jejuni Infections: update on emerging issues and trends". Clinical Infectious Diseases. 32 (8): 1201–1206. doi:10.1086/319760. PMID 11283810.
© MMXXIII Rich X Search. We shall prevail. All rights reserved. Rich X Search