
Back ولادة جنين ميت Arabic Мъртвородено Bulgarian মৃত সন্তান প্রসব Bengali/Bangla Mrtvorođenče BS Mort fetal Catalan Dødfødsel Danish Totgeburt German Muerte fetal Spanish Surnultsünd Estonian مردهزایی Persian
| Stillbirth | |
|---|---|
| Other names | Fetal death, fetal demise[1] |
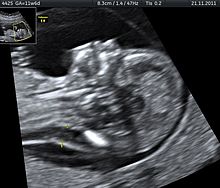 | |
| Ultrasound is often used to diagnose stillbirth and medical conditions that raise the risk. | |
| Specialty | Gynaecology, neonatology, pediatrics, obstetrics |
| Symptoms | Fetal death at or after 20 / 28 weeks of pregnancy[1][2]: Overview tab |
| Causes | Often unknown, pregnancy complications[1][3] |
| Risk factors | Mother's age over 35, smoking, drug use, use of assisted reproductive technology[4] |
| Diagnostic method | No fetal movement felt, ultrasound[5] |
| Treatment | Induction of labor, dilation and evacuation[6] |
| Frequency | 1.9 million (1 for every 72 total births)[7] |
Stillbirth is typically defined as fetal death at or after 20 or 28 weeks of pregnancy, depending on the source.[1][2]: Overview tab, [8] It results in a baby born without signs of life.[9] A stillbirth can often result in the feeling of guilt or grief in the mother.[10] The term is in contrast to miscarriage, which is an early pregnancy loss,[11] and sudden infant death syndrome, where the baby dies a short time after being born alive.[10]
Often the cause is unknown.[1][12] Causes may include pregnancy complications such as pre-eclampsia and birth complications, problems with the placenta or umbilical cord, birth defects, infections such as malaria and syphilis, and poor health in the mother.[2]: Causes tab, [3][13] Risk factors include a mother's age over 35, smoking, drug use, use of assisted reproductive technology, and first pregnancy.[4] Stillbirth may be suspected when no fetal movement is felt.[5] Confirmation is by ultrasound.[5]
Worldwide prevention of most stillbirths is possible with improved health systems.[2]: Overview tab, [14] Around half of stillbirths occur during childbirth, with this being more common in the developing than developed world.[2]: Info panel, Otherwise, depending on how far along the pregnancy is, medications may be used to start labor or a type of surgery known as dilation and evacuation may be carried out.[6] Following a stillbirth, women are at higher risk of another one; however, most subsequent pregnancies do not have similar problems.[15] Depression, financial loss, and family breakdown are known complications.[14]
Worldwide in 2021, there were an estimated 1.9 million stillbirths that occurred after 28 weeks of pregnancy (about 1 for every 72 births).[16] More than three-quarters of estimated stillbirths in 2021 occurred in sub-Saharan Africa and South Asia, with 47% of the global total in sub-Saharan Africa and 32% in South Asia.[17] Stillbirth rates have declined, though more slowly since the 2000s.[18] According to UNICEF, the total number of stillbirths declined by 35%, from 2.9 million in 2000 to 1.9 million in 2021.[16] It is estimated that if the stillbirth rate for each country stays at the 2021 level, 17,5 million babies will be stillborn by 2030.[16]
- ^ a b c d e "Stillbirth: Overview". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ a b c d e "Stillbirth". World Health Organization. Archived from the original on 19 October 2022. Retrieved 29 November 2022.
- ^ a b "What are possible causes of stillbirth?". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ a b "What are the risk factors for stillbirth?". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ a b c "How is stillbirth diagnosed?". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ a b "How do health care providers manage stillbirth?". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ "Stillbirth (UNICEF Data)". UNICEF Data. Retrieved 2023-10-25.
- ^ "What is Stillbirth?". Center of Disease Control and Prevention. Retrieved 17 Sep 2020.
- ^ Bamber AR (2022). "Macerated Stillbirth". In Khong TY, Malcomson RD (eds.). Keeling's Fetal and Neonatal Pathology. Cham: Springer International Publishing. pp. 345–368. doi:10.1007/978-3-030-84168-3_15. ISBN 978-3-030-84168-3. S2CID 245649279.
- ^ a b Robinson GE (January 2014). "Pregnancy loss". Best Practice & Research. Clinical Obstetrics & Gynaecology. 28 (1): 169–178. doi:10.1016/j.bpobgyn.2013.08.012. PMID 24047642. S2CID 32998899.
- ^ Devall AJ, Melo P, Coomarasamy A (2022-03-01). "Progesterone for the prevention of threatened miscarriage". Obstetrics, Gynaecology and Reproductive Medicine. 32 (3): 44–47. doi:10.1016/j.ogrm.2022.01.005. S2CID 246689049.
- ^ Edeib D (29 November 2022). "After a Stillbirth, an Autopsy Can Provide Answers. Too Few of Them Are Being Performed". ProPublica. Retrieved 29 November 2022.
- ^ Lawn JE, Blencowe H, Waiswa P, Amouzou A, Mathers C, Hogan D, et al. (February 2016). "Stillbirths: rates, risk factors, and acceleration towards 2030". Lancet. 387 (10018): 587–603. doi:10.1016/S0140-6736(15)00837-5. PMID 26794078.
- ^ a b "Ending preventable stillbirths An Executive Summary for The Lancet's Series" (PDF). The Lancet. Jan 2016.
- ^ "Stillbirth: Other FAQs". NICHD. 23 September 2014. Archived from the original on 5 October 2016. Retrieved 4 October 2016.
- ^ a b c "Stillbirths". UNICEF Data. Retrieved 2023-10-25.
- ^ "Stillbirths and stillbirth rates". UNICEF DATA. Retrieved 2023-10-31.
- ^ Lawn JE, Blencowe H, Waiswa P, Amouzou A, Mathers C, Hogan D, et al. (February 2016). "Stillbirths: rates, risk factors, and acceleration towards 2030". Lancet. 387 (10018): 587–603. doi:10.1016/S0140-6736(15)00837-5. PMID 26794078.
© MMXXIII Rich X Search. We shall prevail. All rights reserved. Rich X Search