
Back متلازمة خلل التنسج النخاعي Arabic میئلودیسپلاستیک سندرومی AZB Mijelodisplazijski sindrom BS Síndrome mielodisplàstica Catalan Myelodysplastický syndrom Czech Myelodysplastisk syndrom Danish Myelodysplastisches Syndrom German Μυελοδυσπλαστικό σύνδρομο Greek Síndrome mielodisplásico Spanish سندرم میلودیسپلاستیک Persian
| Myelodysplastic syndrome | |
|---|---|
| Other names | Preleukemia, myelodysplasia[1][2] |
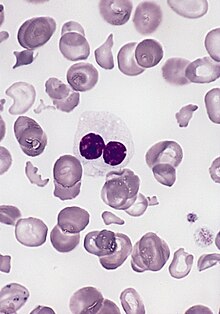 | |
| Blood smear from a person with myelodysplastic syndrome. A hypogranular neutrophil with a pseudo-Pelger-Huet nucleus is shown. There are also abnormally shaped red blood cells, in part related to removal of the spleen. | |
| Specialty | Hematology, oncology |
| Symptoms | None, feeling tired, shortness of breath, easy bleeding, frequent infections[3] |
| Usual onset | ~ 70 years old[4] |
| Risk factors | Previous chemotherapy, radiation therapy, certain chemicals such as tobacco smoke, pesticides, and benzene, exposure to mercury or lead[3] |
| Diagnostic method | Blood test, bone marrow biopsy[3] |
| Treatment | Supportive care, medications, stem cell transplantation[3] |
| Medication | Lenalidomide, antithymocyte globulin, azacitidine[3] |
| Prognosis | Typical survival time 2.5 years[3] |
A myelodysplastic syndrome (MDS) is one of a group of cancers in which immature blood cells in the bone marrow do not mature, and as a result, do not develop into healthy blood cells.[3] Early on, no symptoms typically are seen.[3] Later, symptoms may include fatigue, shortness of breath, bleeding disorders, anemia, or frequent infections.[3] Some types may develop into acute myeloid leukemia.[3]
Risk factors include previous chemotherapy or radiation therapy, exposure to certain chemicals such as tobacco smoke, pesticides, and benzene, and exposure to heavy metals such as mercury or lead.[3] Problems with blood cell formation result in some combination of low red blood cell, platelet, and white blood cell counts.[3] Some types of MDS cause an increase in the production of immature blood cells (called blasts), in the bone marrow or blood.[3] The different types of MDS are identified based on the specific characteristics of the changes in the blood cells and bone marrow.[3]
Treatments may include supportive care, drug therapy, and hematopoietic stem cell transplantation.[3] Supportive care may include blood transfusions, medications to increase the making of red blood cells, and antibiotics.[3] Drug therapy may include the medications lenalidomide, antithymocyte globulin, and azacitidine.[3] Some people can be cured by chemotherapy followed by a stem-cell transplant from a donor.[3]
About seven per 100,000 people are affected by MDS; about four per 100,000 people newly acquire the condition each year.[4] The typical age of onset is 70 years.[4] The prognosis depends on the type of cells affected, the number of blasts in the bone marrow or blood, and the changes present in the chromosomes of the affected cells.[3] The average survival time following diagnosis is 2.5 years.[4] MDS was first recognized in the early 1900s;[5] it came to be called myelodysplastic syndrome in 1976.[5]
- ^ "Myelodysplasia". SEER. Archived from the original on 27 October 2016. Retrieved 27 October 2016.
- ^ "Myelodysplastic Syndromes". NORD (National Organization for Rare Disorders). Retrieved 23 May 2019.
- ^ a b c d e f g h i j k l m n o p q r s "Myelodysplastic Syndromes Treatment (PDQ®) – Patient Version". NCI. 12 August 2015. Archived from the original on 5 October 2016. Retrieved 27 October 2016.
- ^ a b c d Germing U, Kobbe G, Haas R, Gattermann N (November 2013). "Myelodysplastic syndromes: diagnosis, prognosis, and treatment". Deutsches Ärzteblatt International. 110 (46): 783–90. doi:10.3238/arztebl.2013.0783. PMC 3855821. PMID 24300826.
- ^ a b Hong WK, Holland JF (2010). Holland-Frei Cancer Medicine 8 (8 ed.). PMPH-USA. p. 1544. ISBN 9781607950141. Archived from the original on 2016-10-27.
© MMXXIII Rich X Search. We shall prevail. All rights reserved. Rich X Search